Although Arkansas’s population is 16% Black, only about 9% of all COVID-19 vaccine doses administered in the state have gone to Black people. The state is 8% Latino, but under 4% of shots given have been administered to Latinos. Out of the roughly 12,000 Marshallese people who live in Arkansas, just 705 had received a vaccine as of Saturday.Those numbers, retrieved from the Arkansas Department of Health’s COVID dashboard on Friday, are consistent with trends elsewhere. A New York Times analysis of state-level data from March 5 showed COVID vaccination rates among Black and Latino people in all of Arkansas’s neighbors lagged well behind rates for whites.
Arkansas first began publishing demographic data on vaccinations last week, later than most states. It is also incomplete: As of Saturday, the state lacked information about the race of the recipient for more than 10% of shots administered.
The pace of vaccinations in Arkansas is accelerating, with thousands of shots given every day at pharmacies, hospitals and mass clinics across the state. Robert Ator, the retired Arkansas National Guard colonel overseeing the state’s distribution plan, said on Tuesday that the state is now receiving around 92,000 doses of vaccine each week. Over 525,000 people in the state had received at least one dose as of Saturday, and about 291,000 were fully vaccinated. (Most of the vaccines administered thus far require two separate doses to be fully effective; some providers began receiving a new, one-dose version last week.)
But even as the flow of vaccines ramps up, white people seem to be getting shots faster than people of color. Health department spokeswoman Danyelle McNeill said there were multiple reasons for the disparities.
“They include barriers in access to the vaccines, such as lack of internet access, computers, or transportation,” she wrote in an email. “They also include hesitancy in receiving the vaccine because of mistrust in the health system as well as a lack of accurate information.”
Last year, when the vaccine rollout was in its early stages, some national surveys indicated a large percentage of Black people were reluctant to get a shot. That appears to be changing: A recent NPR / Marist poll found similar hesitancy rates among Black and white Americans, with a somewhat higher rate among Latinos. (The poll found a much larger gap by partisan affiliation, with almost half of Republican men saying they were not planning to get vaccinated.)
Access continues to be a problem, especially for people who lack internet access or who do not speak English fluently. The bulk of vaccines in Arkansas are distributed through individual hospitals and pharmacies, many of which do not have translators and often require online signups. (Last week, Governor Hutchinson announced the creation of a new state hotline for vaccine seekers, 1-800-985-6030, which includes bilingual assistance options.) People of color also may be less likely to have flexible work hours, making it harder to schedule an appointment.
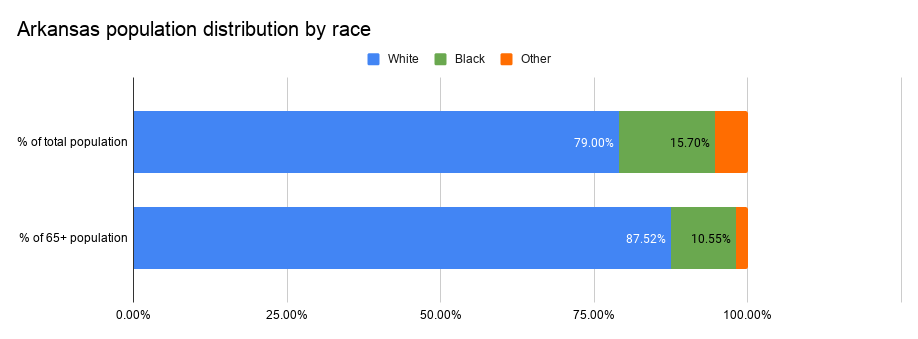
Along with hesitancy and access issues, the disparities may also be driven by the fact that older Arkansans — who were among the first groups eligible for the vaccine — are simply more likely to be white. The state’s population as a whole is about 79% white, but the number increases to 88% for people over age 65.
That is partly because some populations that are relatively new to the state, such as the Latino and Marshallese communities, tend to be younger on average. But it is also because life expectancies are lower among Black Arkansans, the result of health disparities fueled by generations of systemic racism. About 1 in 6 of all Arkansans are Black — but among people age 65 and up, only about 1 in 9 are Black.
As a result, only about 7% of the COVID shots given to people over age 65 have gone to Black residents, according to a health department PowerPoint slide from March 5 provided in response to a Freedom of Information Act request.
“There's a whole lot fewer Black people who survive to live above 70,” said Dr. Gary Wheeler, a a retired infectious disease specialist and former health department official who is familiar with the vaccination data. “In poor counties in the Delta, the life expectancy is 10 years shorter for Black people than it is than it is for largely white counties in Northwest Arkansas. This was one of the first data points where I went, ‘Oh my God, that really does make a huge difference.’ ”
The state is currently in Phase 1-B of its vaccination plan, meaning eligibility is limited to people 65 and older, educators, child care workers, manufacturing and food processing workers, first responders and certain other groups. (Phase 1-A, the first phase, targeted health care workers and residents and staff of nursing homes.) In the coming weeks, the state is expected to move to Phase 1-C, which includes people under 65 with certain underlying health conditions and workers in various other sectors.
Michelle Smith, the health department’s director of the office of health equity, acknowledged that Black people make up a smaller share of the 65-plus group. “That's why it's so critical to open up the phases — so that more of that population is eligible,” she said.
(Racial disparities persist among seniors even on a proportional basis, according to a slide provided by the health department. As of Thursday, 25% of white residents age 65 and up were fully vaccinated, compared to just 16% of Black residents and 12% of Latinos in the same age group. The gap was smaller among those who had received their first dose.)
However, opening up eligibility too quickly could also impede the state’s efforts to address equity concerns. Ator, the state’s vaccine distribution chief, said the overall supply of doses remains limited. If too many eligible people are seeking shots at the same time, that could make it harder to allocate doses for specific communities and events.
“It's very simple — if you open it up, and the demand is [high] in every corner of the state, then you have less capacity by way of supply to address these needs,” he said.
Currently, he said, the state dedicates about 70% of the vaccine it receives each week to provide a baseline amount of doses to pharmacies and hospitals. The other 30% is allocated on a rolling basis — some for mass events, some for specific workforces, some for additional doses to providers in specific places.
“It allows [us] to dedicate doses for the minority community,” he said. “It allows [us] to facilitate mass events without disrupting that consistent flow of vaccine going out to all the different counties. What we're trying to do is provide a nice, consistent answer for how we're going about this. And if you just open it wide open, I mean, it becomes the Hunger Games.”
Since January, Smith said, her office has organized “strike teams” to quickly deliver large volumes of doses to minority communities with lagging rates of vaccination.
“We look at where counties have the lowest percentages of African-Americans or Latinos receiving the vaccine, and we put together a mass vaccination clinic,” she said. With the help of local leaders and medical providers, the health department has organized 10 such events since the end of January, administering around 6,000 doses. This week, the department also began scheduling large vaccination events at local health units around the state.
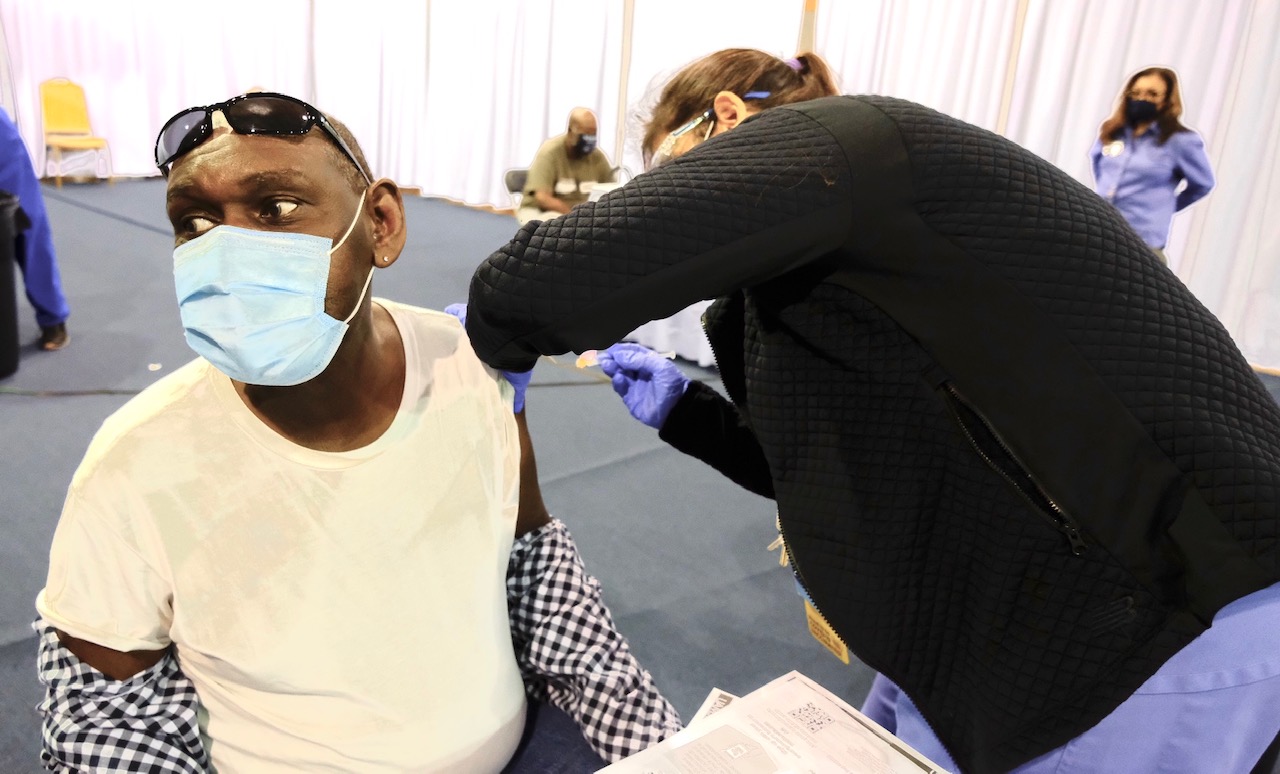
On Friday, the city of Pine Bluff held its second mass clinic at the Pine Bluff Convention Center, in partnership with the health department and Doctor’s Orders, a local pharmacy. Mary Liddell, the city’s community outreach coordinator, said a team of some 135 volunteers and staff administered more than 750 shots over the course of the day.
“This is very much needed. With the pharmacists, there’s just so many that they can take in,” she said, speaking to a reporter between shifts at the Friday clinic. “For us to set this up in the convention center, it’s going to reach the masses, so to speak.”
Ator said Jefferson County, where Pine Bluff is located, has been a success story. “We have worked really, really hard down in that area,” he said. “It’s not good enough just to dump vaccine in a county. You have to work with community leaders — they're the ones that give you the access to that community, to where [people] trust and are comfortable with what we’re doing.”
Some advocates, though, say the state is falling behind elsewhere. Mireya Reith, the director of Arkansas United, an immigrant advocacy organization, said Latino, Marshallese and other minority communities are in need of help with the signup process.
The creation of a hotline with a Spanish language option was “definitely an improvement,” Reith said, “but that’s not where people get information.” What’s needed, she said, is funding for navigators to help people sign up for appointments directly.
Last summer, when coronavirus cases and deaths surged among Latino and Marshallese residents of Northwest Arkansas, the state began directing federal relief money toward testing, contact tracing and other services in those communities. But, Reith said, much of that federal money disappeared at the end of 2020 and has yet to be replaced.
“We had a lot of help when the numbers went up, but it's like the state just keeps waiting for the worst case scenario before taking action,” she said.
This reporting is courtesy of the Arkansas Nonprofit News Network, an independent, nonpartisan news project dedicated to producing journalism that matters to Arkansans.